Holmium Laser Enucleation of the Prostate (HoLEP) Guide
The common symptoms that accompany an enlarged prostate gland can cause emotional as well as physical distress, but when lifestyle changes are not enough to tackle the problem, a minimally invasive surgical technique is offering hope for men to get their lives back on track
An enlarged prostate gland is one of the most common medical conditions affecting men as they grow older.
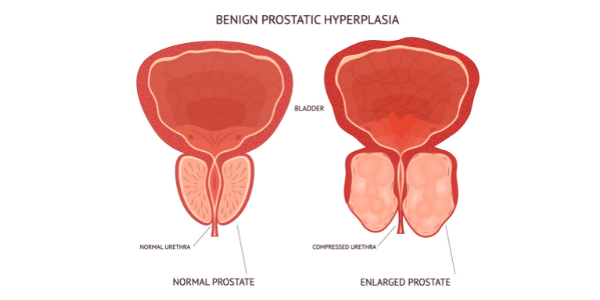
Indeed, it is estimated that as many as half of all men over the age of 50 have some degree of prostate enlargement – known clinically as benign prostatic hyperplasia (BPH). And, in the over-80s, that figure shoots up to more than 80%.
A normal prostate typically weighs in at around 30 grams, but the hormonal changes that occur with age can cause it to grow dramatically – to in excess of 80 grams in the most severe cases.
The resulting pressure on the bladder and the urethra can lead to a host of symptoms many men will find familiar. Hesitancy, increased frequency – especially at night – and weak urine flow are all common in middle age. These can often be improved with simple lifestyle changes. However, progressive BPH can result in a range of more worrying lower urinary tract problems, such as blood in the urine, incomplete bladder emptying and repeated infection.
Although BPH is not cancerous, serious complications can arise if it is left untreated, including urinary retention – a painful condition where the prostate blocks the urine flow completely and which requires emergency treatment.
When would you need HoLEP?
Mr Marios Hadjipavlou, consultant urological surgeon at the world-renowned King Edward VII’s Hospital in London, recommends men always get their symptoms checked by a doctor.
‘A PSA blood test and simple physical examination is often enough to rule out something more sinister, such as cancer,’ says Mr Hadjipavlou. ‘Sometimes an MRI will be needed and, less frequently a biopsy will be required, but this can be done very easily through the skin, transperineal and under a local anaesthetic or sedation.’
If BPH is identified as the problem, there are a variety of treatment options. Conservative management can often be enough to tackle mild symptoms. More progressive forms of the condition can be treated with medication but for particularly enlarged prostates or in cases where patients cannot tolerate medication, surgery might be needed.
This can feel like a daunting prospect, but advances in minimally invasive surgical techniques are leading to faster recovery times, fewer side effects and better outcomes for patients – even those with progressive BPH.
How does HoLEP work?
Mr Hadjipavlou specialises in endourology, which unlike classical open surgery, uses small, thin instruments passed through the urethra to perform surgery without the need for incisions. There are a number of minimally invasive techniques available to treat moderate BPH, but at King Edward VII’s Hospital, he is advancing the use of holmium laser enucleation of the prostate, known as HoLEP, to treat the most complex cases.
Holmium lasers have long been used in the treatment of kidney stones. However, their use in treating prostate enlargement is confined to just a few specialist centres. The technique itself is complex and takes time to master. Currently, Mr Hadjipavlou is one of just a handful of surgeons able to offer HoLEP in London.
‘HoLEP is beneficial for patients that have larger prostates because other techniques can’t remove as much of the excess tissue and so do not work particularly well for patients with very enlarged prostates. There is also limited availability in the UK, so while HoLEP can be used to treat smaller prostate enlargement, it is generally reserved for people that have a prostate larger than 70 or 80 grams and, therefore, fewer treatment options,’ explains Mr Hadjipavlou.
HoLEP Procedure
The procedure itself is carried out under general anaesthetic and can usually be completed in around an hour – sometimes longer if the prostate is particularly enlarged. Mr Hadjipavlou describes it a bit like making a hole in an orange and peeling it from the inside.
‘We insert a fine telescope through the urethra and essentially carve out the inner, enlarged part of the prostate with a laser device which cuts and controls bleeding at the same time,’ he says.
A power morcellator device is then used to ‘mince’ the excess tissue, allowing it to be removed through the bladder and out through the urethra.
‘Because there are no knives and no incisions, patients won’t experience any pain,’ says Mr Hadjipavlou. ‘They will require an overnight stay in hospital and a catheter will be inserted immediately at the end of the operation, but this is usually removed the next morning and they will be able to pee normally straight away.’

The benefits can outweigh the risks
Patients often experience some mild post-operative symptoms such as burning, urgency and frequency following the procedure, but these generally improve over two to three weeks.
‘The benefits for men following surgery are enormous,’ says Mr Hadjipavlou. ‘Their flow and bladder emptying will immediately be massively better and after six weeks they can expect to be back to normal.’
No surgery is without risk and there is a possibility of temporary urinary leakage, which can become long term in rare cases, and narrowing of the urethra – although this can usually be managed by a gentle stretching procedure in most cases.
There is also a small risk of erectile dysfunction, but it is common for men to lose their ability to ejaculate. Because HoLEP is generally performed for advanced prostate enlargement, which tends to affect older men, this is often not a problem, but Mr Hadjipavlou says those wishing to preserve their fertility will need to consider carefully before deciding whether it is the right choice for them.
However, for most men suffering symptoms of advanced prostate enlargement, the benefits far outweigh the risks. And advances in laser technology as well as surgical techniques are providing enhanced outcomes for patients.
Mr Hadjipavlou uses the pioneering the en-bloc technique where the excess prostate tissue is detached in one piece, making the operation much faster with low risk of urinary incontinence. Since almost all of the excess tissue is removed with HoLEP, it is rare for it to grow back, meaning that patients usually require no further treatment for the rest of their lives.
‘As well as immediate relief from symptoms, in the long-term men will have a lower risk of urinary infection and blood in the urine,’ he says. ‘But the first thing that many patients say when we follow them up is that they are peeing like a 20-year-old and that can make a massive difference to their lifestyle as well as their confidence.’
More information
- If you’re concerned about your prostate health, make an appointment to see your GP, who can refer you to a specialist for testing. (Don’t have a GP?)
- Find out more about King Edward VII’s Hospital’s Urology Department and speak to a specialist today