Health Hub
Life after breast cancer

Receiving the all clear after breast cancer treatment marks the end of a long journey of therapies and possibly surgery. It can leave you with a mix of emotions ranging from relief to a fear of the unknown. Some people also describe the feeling as one of loss, after such a long and regular timetable of appointments and treatments.
Adjusting to life as a breast cancer survivor can be difficult, not least because there may be decisions you still need to make. These involve potential nipple micropigmentation, physiotherapy, managing the possibility of lymphoedema and genetic testing.
Therapies starting, or being aware of them, as early as possible, even before your treatment ends, will help to support your recovery and restoration.
If your treatment has now finished, you’re perhaps thinking, what next? Or, you may still be in treatment and interested to know what happens after you’ve had surgery or your last chemotherapy or radiotherapy session.
It’s completely normal to feel lost or unsure on what to do next to aid your recovery and build your confidence and self-esteem. Here, we talk to breast clinical nurse specialists, physiotherapists and genetic counsellors from King Edward VII’s Hospital Breast Unit to help you navigate the next steps in your recovery.

Nipple micropigmentation
Nipple reconstruction with micropigmentation is an empowering procedure that you can decide to have after breast surgery to create the illusion of a nipple. King Edward VII’s Hospital Breast Service Manager, Amelia Cook, explains more.
What is nipple micropigmentation?
Sometimes, it’s necessary to remove the nipple as part of breast cancer surgery for your safety. Nipple micropigmentation is a semi-permanent tattooing technique to give the impression of a nipple areola complex. Modern breast reconstruction surgery gives a very natural look – nipple micropigmentation can also look very realistic and for some, is the final step in reconstruction.
Prior to surgery, you will speak to a specialist that can talk you through how it may look for you and what your choices are. You can then review and refine your choices after surgery.
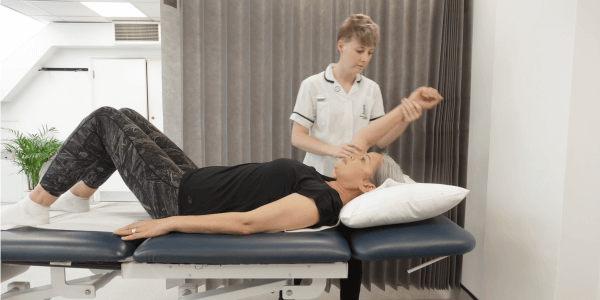
Physiotherapy after breast cancer surgery
Physio can be a helpful therapy during your recovery from surgery to help prevent or manage mobility problems in your arms and shoulders and to improve problems caused by tight scarring. Specialist Physiotherapist for the King Edward VII’s Hospital, Jenny Earl, talks about the benefits of physiotherapy following breast cancer surgery.
Why might I need physio after surgery for breast cancer?
Physiotherapy can help to prevent long term problems with shoulder movement, posture and lymphoedema and can help to support your return to your normal activities and sport. It can also help to relieve discomfort caused by tight scarring, and the formation of tight, rope-like structures called cording.
How does physio help?
Physiotherapy sessions include a range of exercises designed to increase your range of movement, and it’s a very individualised approach. Each patient is different, with differences in lifestyle, starting point and surgery. You may also have an increased risk of shoulder problems following surgery if you already had stiffness or pain in your shoulder.
For these reasons, physiotherapy is very patient-centred and individual. It normally begins with very low level, below shoulder height exercises. Depending on how you’re healing, as an outpatient and when you’re safe to progress, you will then move to an increased level of movement to support your return to general exercise.
Exercise is important for your general health and wellbeing, and your physiotherapist will find a way to incorporate exercise into your recovery, completely at your own pace.
Once you’ve regained or maintained a range of movement within your shoulder, your physio will introduce strength exercise to aid your return to full function.

Lymphoedema following breast cancer surgery
The lymphatic system is a network of channels that spread throughout the body to carry a clear fluid called lymph. Lymph forms part of the immune system and helps to fight infections and drain excess fluid from the body.
When this system isn’t working properly, it can cause a build up of fluid, leading to swelling and lymphoedema. King Edward VII’s Hospital lymphoedema expert Ashleigh Jordan explains why this can affect people following breast surgery, and how it can be managed.
What is lymphoedema?
During breast cancer surgery, some or all of the lymph nodes in the armpit are removed. When this happens, the flow of lymph fluid is disrupted, which can cause fluid to collect and lead to swelling in the arm – this is called lymphoedema.
Lymphoedema affects around 2 in 10 people following breast cancer surgery, with the risk higher in those with multiple lymph nodes removed. It can also follow radiotherapy that can cause scarring and blockages in the lymph nodes in the armpit. Lymphoedema can happen at any point following surgery or radiotherapy, and the risk remains for the rest of a patients’ life.
The condition can be very upsetting, and cannot be cured. However, physiotherapy can help to manage it.

Genetic testing for breast cancer
With the advancements of science, genetic testing is now quicker and cheaper, with results becoming available within weeks, rather than months or even longer.
Availability is also better now, and since Angelina Jolie revealed that she had the BRCA1 gene mutation that gave her a significantly increased risk of developing both breast and ovarian cancer, there has been a much larger awareness of genetic testing for cancer.
Knowing if we have a genetic mutation can help to guide treatment and inform family members of their own risk. Here, King Edward VII’s Hospital consultant, Dr Ananja Kulkarni explains more.
What is genetic testing for breast cancer and why might I need it?
Most breast cancer is sporadic – this means that most of the time, no genetic cause can be found, and is more likely to have hormonal or environmental links, or be due to other, unknown, genetic factors.
In fact, only around 3-5% of breast cancers are due to an underlying, inherited mutation, or variant, in a gene, that is, a genetic mutation that can lead to breast cancer that is inherited from a family member.
However, there are factors associated with a potential genetic link and could be a sign of inherited cancer, and these include:
- Being diagnosed below the age of 40 or before the menopause
- Breast cancer affecting both breasts (particularly under the age of 50)
- Clustering – close family members with breast or a related cancer such as ovarian, prostate or pancreatic cancer
- Having two separate types of cancer
- Being part of certain communities or having certain ancestry, for example people with Ashkenazi Jewish heritage have a higher prevalence of the BRCA1 and 2 genes
These factors mean that family testing for an inherited gene could be helpful.
When the treatment ends: Life after breast cancer
When your breast cancer treatment finishes, there’s no need to feel lost or overwhelmed. At the King Edward VII’s Hospital, we have a team of specialists offering integrative care to help you improve your quality of life after being diagnosed with breast cancer.
Your body image is central to giving you confidence and we can help you navigate the minefield of options that will best support your care and your needs.
You can make an appointment via a self-referral to see us at any point in your journey. Or, you can organise a chat over Zoom to see how we can help you. You don’t need to have had surgery with us to book ongoing support.
Watch our informative Life After Breast Cancer webinar to learn how our multidisciplinary team can help provide you with an individualised care plan post-breast cancer treatment to support your recovery.
More information
- The Breast Unit at King Edward VII’s Hospital has clinical nurse specialists, breast care nurse specialists, consultant radiologists, psychologists, pain and comfort management specialists, holistic healing partners and physiotherapists offering before and after surgery treatments.
- We offer breast screening, breast cancer treatment, breast reconstruction, nipple micropigmentation, physiotherapy for breast cancer related frozen shoulders and cording and genetic screening.
- We also offer all inclusive breast screening packages for those under 40 years old and 40+ years old.
Article Sections
Latest Hospital News
Should you wish to speak to our press team, please visit Press Enquiries




